Impact Factor ISSN: 1837-9664
J Cancer 2022; 13(2):602-609. doi:10.7150/jca.64335 This issue Cite
Research Paper
Upfront brain radiotherapy improves intracranial progression-free survival but not overall survival in lung adenocarcinoma patients with brain metastases: a retrospective, single-institutional analysis from China
1. Department of Radiation Oncology, Shandong Cancer Hospital, Shandong University, Jinan, 250117, Shandong, China.
2. Department of Radiation Oncology, Qingdao University Medical College Affiliated Yantai Yuhuangding Hospital, Yantai, 264000, Shandong, China.
3. Department of Radiation Oncology, Affiliated Hospital of Xuzhou Medical University, Xuzhou, 221002, Jiangsu, China.
Abstract
Aims: The optimal timing of brain radiotherapy (BRT) for lung adenocarcinoma patients with brain metastases (BM) remains controversial. In this retrospective study, we performed a retrospective review to investigate the differential benefit of upfront versus deferred BRT for lung adenocarcinoma patients with BM.
Methods: A total of 354 lung adenocarcinoma patients with BM treated in the Affiliated Cancer Hospital of Shandong University met the inclusion criteria for the study. Patients were divided into two groups: upfront BRT and deferred BRT. Intracranial progression-free survival (PFS) and overall survival (OS) were measured from the date of brain metastases. Subgroup analyses according to gene mutation status were also performed.
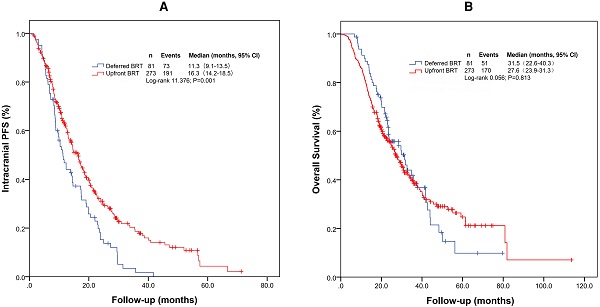
Results: Among the entire cohort, the median intracranial PFS with upfront BRT (16.3 months) was longer than that with deferred BRT (11.3 months, p=0.001). However, the median OS did not differ significantly between patients who received upfront BRT and deferred BRT (27.6 and 31.5 months, respectively, p=0.813). Subgroup analyses indicated that upfront BRT yielded a significantly longer intracranial PFS than deferred BRT (p=0.003) for patients without EGFR (19 or 21) mutation. In both subgroups, the median OS showed no significant difference between upfront BRT and deferred BRT.
Conclusion: This single-institutional retrospective study showed that in lung adenocarcinoma patients with brain metastases, upfront BRT was associated with a significantly longer intracranial PFS but not improvement in OS compared with deferred BRT. Considering the neurocognitive toxicities of BRT previously reported in the literature, deferred BRT might be considered as an acceptable therapeutic option for the treatment of patients with lung adenocarcinoma and BM.
Keywords: brain metastases, lung adenocarcinoma, epidermal growth factor receptor, tyrosine kinase inhibitor, brain radiotherapy

 Global reach, higher impact
Global reach, higher impact