Impact Factor ISSN: 1837-9664
J Cancer 2021; 12(6):1734-1741. doi:10.7150/jca.51212 This issue Cite
Research Paper
Para-aortic lymph node metastasis in lower Thoracic Esophageal Squamous Cell Carcinoma after Radical Esophagectomy: a CT-based atlas and its clinical implications for Adjuvant Radiotherapy
1. Department of Radiation Oncology, Fudan University Shanghai Cancer Center, Shanghai 200032, China.
2. Department of Oncology, Shanghai Medical College, Fudan University, Shanghai 200032, China.
3. Department of Radiology, Fudan University Shanghai Cancer Center, Shanghai 200032, China.
4. Department of Medical Oncology, the Second Affiliated Hospital of Kunming Medical University, Yunnan 650101, China.
5. Institute of Thoracic Onology, Fudan University, Shanghai 200032, China.
#Co-first authors with equal contributions to this work.
Abstract
Background: Our previous work showed that para-aortic lymph node (PALN) metastasis was the major failure pattern in lower thoracic esophageal squamous cell carcinoma (LTESCC) patients who presented abdominal LN failure after curative surgery. We thereby aim to generate a computerized tomography (CT)-based documentation of PALNs and to propose a clinical target volume (CTV) for this region.
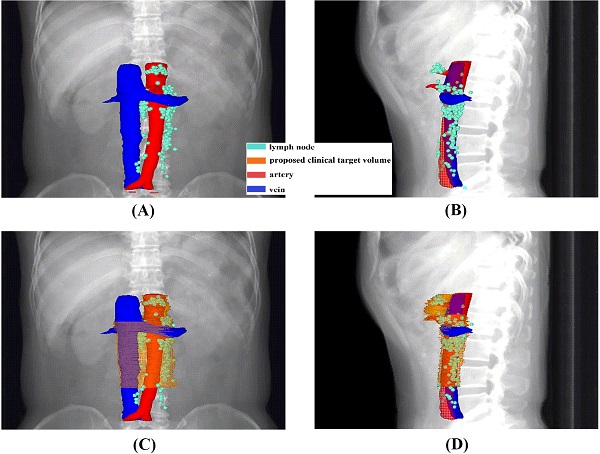
Methods: Sixty-five patients were enrolled. The epicentre of each PALN was drawn onto an axial CT image of a standard patient with reference to the surrounding anatomical landmarks. A CTV for PALN was generated based on the final result of node distribution, and was evaluated for dosimetric performance in three simulated patients.
Results: All the studied 248 LNs were below the level of 1.0 cm above the celiac artery (CA), and 94.76% were above the bottom of vertebra L3. Horizontally, 93.33% of the LNs in the celiac level were located within an expansion of 1.5 cm on the CA, and 94.12% of the LNs in the superior mesenteric artery (SMA) level were within 1.5 cm on the left side of the SMA. Below the SMA, all the LNs were behind the left renal vein, left to the right border of the inferior vena cava, and 98.51% of the LNs were medial to the lateral surface of the left psoas major. The proposed CTV could cover 92.74% of the LNs and was dosimetrically feasible.
Conclusions: The proposed CTV is the first one to focus on the high-risk area of abdominal failure in LTESCC patients after surgery and can serve as a reference in the adjuvant radiotherapy for LTESCC patients.
Keywords: esophageal squamous cell carcinoma, adjuvant radiotherapy, radiation therapy, lymph node, computed tomography

 Global reach, higher impact
Global reach, higher impact