Impact Factor ISSN: 1837-9664
J Cancer 2023; 14(11):2145-2151. doi:10.7150/jca.85939 This issue Cite
Research Paper
Surgical results and quality of life after single-stage posterior transpedicular approach for circumferential epidural decompression in patients with thoracolumbar spine metastasis
Musculoskeletal Tumor Centre, Peking University People's Hospital, 11# Xizhimen South Road, Xicheng District, Beijing, China, 100044.
* These authors contributed equally to this study.
Abstract
Objective: The primary aim of this study was to evaluate the effect of palliative surgery using posterior transpedicular approach (PTA) with posterior instrumentation on pain response and quality of life (QoL) in patients with metastatic thoracic and lumbar tumors.
Methods: From 2018 to 2019, 39 patients with metastatic thoracic and/or lumbar tumors were prospectively enrolled to measure the reduction in pain and the changes in QoL after surgical decompression with posterior instrumentation via PTA. The patient group was composed of 27 men and 12 women with a mean age of 60 years (range, 28 to 92 years). Pain response was measured using the visual analog scale (VAS) and neurologic status was evaluated using Frankel grades. QoL was assessed with use of the EORCT QLQ-BM22 questionnaire before surgery (baseline) and at 1-, 3-, 6-, and 12-month after surgery. The survival times of all the patients were also collected.
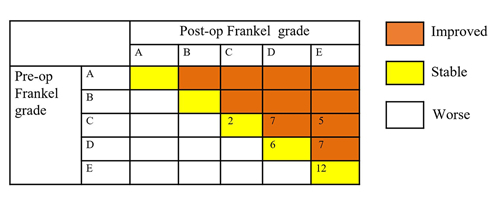
Results: All patients showed either an improvement or a similar pain level after surgery, which the VAS score decreased from 7.10 ± 2.22 preoperatively to 3.10 ± 2.15 one month postoperatively (P<0.05). 19 patients (48.7%, 19/39) showed neurological function improvement postoperatively. Among the 19 patients, 7 cases improved from Frankel grade C to D, 5 cases from grade C to E, and 7 cases from grade D to E. Another 20 patients still have the same Frankel grade postoperatively, however, most of them improved clinically. The QoL improvement of the patients was also evident after treatment. Paired-samples T-test examination of the postoperative scores showed a significant improvement in terms of pain location, pain severity and performance status (P<0.01). Compared with the preoperative score, the 1-month postoperative score of functional interference was significantly improved (63.6 vs. 34.5, P<0.01). There were no significant changes in social or psychological functioning. Three patients experienced cerebrospinal fluid leakage postoperatively, and they were all successfully managed by lying flat without a pillow. One patient experienced rod breakage, at 10 months after surgery. All the patients were alive at 3 months; however, 7 patients died within 3 to 6 months, and another 9 patients died from the disease within 6 to 12 months.
Conclusions: The present feasibility study found that the application of the PTA for decompression and fusion in patients with spinal metastases is beneficial for achieving prompt and sustained pain relief, reducing neurologic deficits and improving functional outcomes, health utilities, and HRQoL.
Keywords: spinal metastases, surgery, quality of life

 Global reach, higher impact
Global reach, higher impact