Impact Factor ISSN: 1837-9664
J Cancer 2021; 12(23):7167-7176. doi:10.7150/jca.60601 This issue Cite
Research Paper
Prevalence of genotype-specific human papillomavirus in cytology specimens and cervical biopsies, and its implication in cervical cancer risk stratification: a retrospective study of 10647 cases
1. Department of Pathology, Zhejiang University School of Medicine Women's Hospital, Hangzhou, Zhejiang Province, 310006, China.
2. Reproductive Medicine Center, Zhongshan City People's Hospital, Zhongshan, Guangdong Province, 528403, China
3. Department of Pathology, Northwestern University, Feinberg School of Medicine, Chicago, IL, 60611, USA.
4. Department of Pathology, University of Texas Southwestern Medical Center, Dallas, TX, 75390, USA.
# Authors contributed equally to this article.
Abstract
Objective: This study aimed to describe the risk stratification of squamous cell carcinoma (SCC) and its precursor lesions based on HPV E6/E7 mRNA genotyping.
Methods: 10647 hrHPV+ women (mean age 40.8 years), who had concurrent cytology and follow-up biopsy results available between September 2016 and May 2020, met the inclusion criteria and were selected for immediate risk analysis.
Results: In this cohort, HPV-16 or 18/45+ women had significantly higher immediate risk of cervical cancer and precancer compared with other genotypes+ women. The relative immediate risk (RIR) of ASC-H+ was 2.0 (95% CI: 1.9-2.4) and SCC was 9.4 (95% CI: 5.5-15.6) for HPV-16 or 18/45+ women when compared with women positive for other 11 genotypes. Among follow-up biopsy cases, the RIR of CIN2+ was 2.7 (95% CI: 3.0-3.7) and SCC was 10.8 (95% CI: 7.2-17.4) for HPV-16 or 18/45+ women than women positive for other genotypes. Similarly, when compared with women positive for other genotypes, the RIR of CIN2+ was 2.9 (95% CI: 2.7-4.6) and SCC was 13.8 (95% CI: 3.0-66.2) for HPV-16 or 18/45+ women with ASC-US, and RIR of CIN2+ was 3.3 (95% CI: 3.1-4.6) and SCC was 22.3 (95% CI: 2.8-176.8) for HPV-16 or 18/45+ women with NILM.
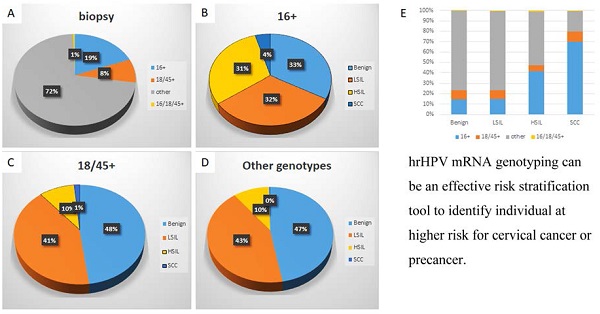
Conclusions: This study supports that hrHPV mRNA genotyping can be an effective risk stratification tool to identify individual at higher risk for cervical cancer or precancer, and provides important evidences for the future modifications for current China cervical cancer screening guidelines.
Keywords: Risk stratification, Cervical screening, Cancer, Human papillomavirus, E6/E7 mRNA genotyping

 Global reach, higher impact
Global reach, higher impact