Impact Factor
ISSN: 1837-9664
J Cancer 2021; 12(22):6749-6755. doi:10.7150/jca.63184 This issue Cite
Research Paper
Risk of Stroke in Patients with Breast Cancer and Sleep Disorders
1. Department of Internal Medicine, Chi Mei Medical Center, Chiali, Tainan, Taiwan.
2. Department of Biotechnology and Food Technology, Southern Taiwan University of Science and Technology, Tainan, Taiwan.
3. Division of Gastroenterology & General Surgery, Chi Mei Medical Center, Tainan, Taiwan.
4. Department of Health and Nutrition, Chia Nan University of Pharmacy and Science, Tainan, Taiwan.
5. Department of Medical Research, Chi Mei Medical Center, Tainan, Taiwan.
6. Department of Anesthesiology, Chi Mei Medical Center, Tainan, Taiwan.
7. Department of Anesthesiology, National Defense Medical Center, Taipei, Taiwan.
8. Department of Information Management, Southern Taiwan University of Science and Technology, Tainan, Taiwan.
9. Cancer Center, Wan Fang Hospital, Taipei Medical University, Taipei, Taiwan.
10. Department of Emergency Medicine, Chi-Mei Medical Center, Tainan, Taiwan.
*Co-first authors that contributed equally to this paper.
Abstract
Breast cancer and stroke were leading cause of cancer-related mortality in the world. Stroke is the second leading cause of death. Previous studies showed that patients with breast cancer had a relatively higher risk of sleep disorders. Sleep disorders increased the risk of stroke. The aim of our study was to examine the risk of stroke after a breast cancer with sleep disorder among women in Taiwan.
The Taiwan Cancer Registry was used to identify patients with breast cancer. Patients with new-onset breast cancer from January 2007 to December 2015 were selected for this study and followed until December 31, 2017. Patients who were diagnosed with sleep disorders were set as the case group, and the controls were those without sleep disorders.
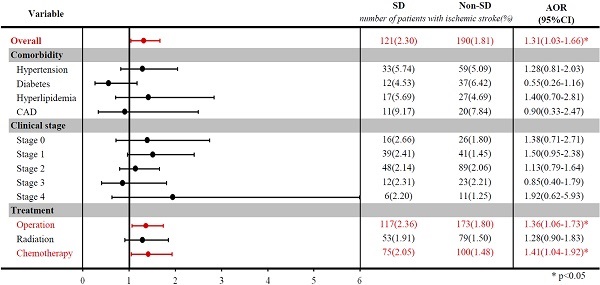
We enrolled 5256 patients with sleep disorders and 10,512 patients without sleep disorders. There were 121 (2.30%) patients with ischemic stroke among the breast cancer patients with sleep disorders. The mean time from the diagnosis of breast cancer to the occurrence of ischemic stroke was 6.29±2.59 years for breast cancer patients with sleep disorders and 6.00±2.76 years for those without sleep disorders (p < 0.0001). After matching by age and index year, breast patients with sleep disorders had a 1.31-fold higher risk (95% confidence interval: 1.03-1.66; p-value=0.026) of ischemic stroke than those without sleep disorders, after adjustment for comorbidities, cancer clinical stage, and treatment types. In conclusion, Breast cancer patients with sleep disorders have an increased risk of stroke.

 Global reach, higher impact
Global reach, higher impact