Impact Factor ISSN: 1837-9664
J Cancer 2021; 12(11):3180-3189. doi:10.7150/jca.50108 This issue Cite
Research Paper
Adjuvant Radiotherapy of Involved Field versus Elective Lymph Node in Patients with Operable Esophageal Squamous Cell Cancer: A Single Institution Prospective Randomized Controlled Study
1. Institute of Modern Physics, Chinese Academy of Sciences, Lanzhou R.P China, 730000.
2. Lanzhou Heavy Ion Hospital, Lanzhou R.P China, 730000.
3. University of Chinese Academy of Sciences, Beijing R.P China, 100049.
4. Gansu Provincial Cancer Hospital, Lanzhou R.P China, 730050.
5. Center of Evidence Based Medicine, Lanzhou University, Lanzhou R.P China, 730000.
*Co-first authors with equal contributions to this work.
Abstract
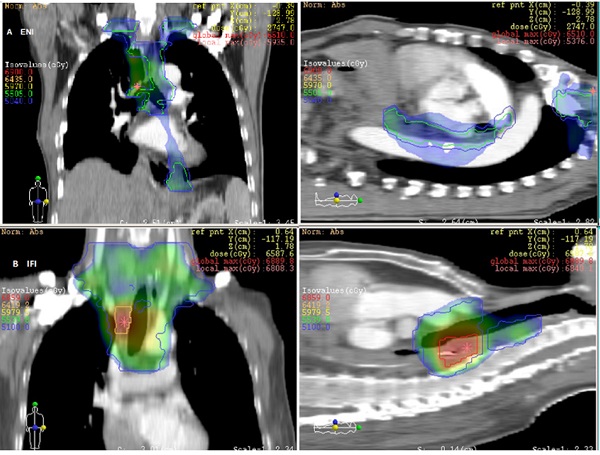
Background: To evaluate locoregional failure and its impact on survival by comparing involved field irradiation (IFI) with elective lymph node irradiation (ENI) for patients with esophageal squamous cell cancer who underwent post-operative radiotherapy.
Methods and Materials: The enrolled patients were randomized allocated to IFI or ENI group. CTV of IFI was generated according to pre-operative primary tumor location and post-operative pathological characters and positive LNs regions. CTV of ENI was generated according to pre-operative tumor position to administer selective lymph node irradiation. Radiotherapy planning was delivered using either 3D-CRT or IMRT.
Results: A total of 57 patients were enrolled, 28 patients in ENI group and 29 patients in IFI group. There were not statistical differences between two groups in baseline (p>0.05). The initial locoregional failure rate was 17.9 % in ENI arm and 20.7% in IFI arm respectively (p=0.085). The 1-, 3-, and 5-year Progression-free Survival (PFS) were 63.2, 43.5, and 21.8 % in ENI arm versus 78.2, 60.1, and 55.1% in IFI arm (p =0.038). The 1-, 3-, and 5-year overall survival (OS) were 78.6, 46.9, and 23.5 % in ENI arm versus 72.9, 59.7, and 54.3 % in IFI arm (p=0.06). Acute radiation pneumonitis (p=0.005) and hematological toxicities (p =0.029) also showed statistical differences between groups, ENI arm was more than IFI arm.
Conclusions: The results indicated that IFI tended to improve survival and reduce toxicities for patients with operative ESCC and did not increase locoregional failure compared to ENI. It is thus suggested that IFI for ESCC PORT is worthy of clinical recommendation and further study.
Keywords: esophageal cancer, lymph node, radiotherapy, clinical outcomes, adjuvant treatment

 Global reach, higher impact
Global reach, higher impact