Impact Factor
ISSN: 1837-9664
J Cancer 2021; 12(7):2113-2121. doi:10.7150/jca.47552 This issue Cite
Research Paper
Laparoscopic gastrectomy reduces adverse postoperative outcomes and decreases morbidity for gastric cancer patients with visceral obesity: a propensity score-matched analysis
1. Department of Gastrointestinal Surgery, The Second Affiliated Hospital, Wenzhou Medical University, Wenzhou, Zhejiang, China.
2. Department of Gastrointestinal Surgery, The First Affiliated Hospital, Wenzhou Medical University, Wenzhou, Zhejiang, China.
3. Department of Medical Microbiology and Immunology, Basic Medical College, Wenzhou Medical University, Wenzhou, Zhejiang, China.
#These authors contributed equally to this work.
Abstract
Background: Laparoscopic gastrectomy for gastric cancer shortens the recovery period without decreasing long-term survival. However, clinical evidence on whether laparoscopic radical gastrectomy reduces the surgical stress and improves the short- and long-term outcomes of obese patients with gastric cancer is lacking. We compared the short- and long-term outcomes of gastric cancer patients with visceral obesity (VO) who underwent laparoscopic gastrectomy (LG) or open gastrectomy (OG).
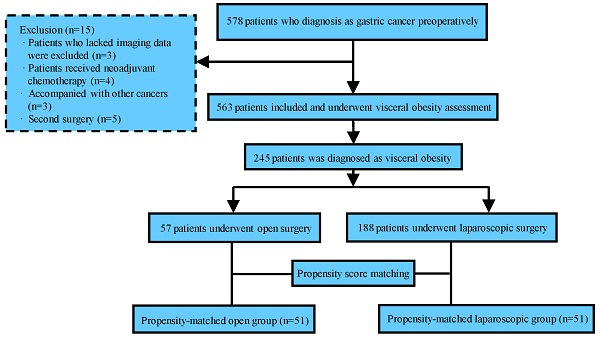
Methods: We prospectively collected data from 578 patients who underwent radical gastrectomy in two centers between January 2014 and December 2016. The visceral fat area (VFA) was measured on the umbilicus level, and VFA ≥100 cm2 was defined as VO. The section bias was reduced by conducting a propensity score matching analysis. The short- and long-term outcomes were further compared between patients who underwent OG and those who underwent LG.
Results: Overall, 245 patients (42.61%) were classified as having VO, of whom 102 were included for further analysis after matching. There were no significant differences in clinical characteristics between the two groups in the matched cohort. The LG group had significantly fewer overall complications (P<0.001) and shorter postoperative hospital stays (P<0.001). Subgroup analysis of postoperative complications also showed that the incidence of surgical complications was lower in the LG group (P=0.002). Further survival analysis showed the LG group had significantly better long-term overall survival (P=0.017).
Conclusions: Compared with open radical gastrectomy, laparoscopy would reduce the rate of postoperative complications in patients with VO, as well as prolong their overall survival.
Keywords: obesity, abdominal, laparoscopy, stomach neoplasms, postoperative complications, survival

 Global reach, higher impact
Global reach, higher impact