Impact Factor
ISSN: 1837-9664
J Cancer 2023; 14(9):1553-1561. doi:10.7150/jca.83588 This issue Cite
Research Paper
A novel nomogram based on clinical blood indicators for prognosis prediction in curatively resected esophagogastric junction adenocarcinoma patients
1. Department of Clinical Laboratory Medicine, Cancer Hospital of Shantou University Medical College, Shantou 515041, Guangdong, China.
2. Esophageal Cancer Prevention and Control Research Center, Cancer Hospital of Shantou University Medical College, Shantou 515041, Guangdong, China.
3. Guangdong Esophageal Cancer Research Institute, Guangzhou 510060, Guangdong, China.
4. Department of Gastrointestinal Endoscopy, First Affiliated Hospital of Shantou University Medical College, Shantou 515041, Guangdong, China.
5. Department of Head and Neck Surgery, Cancer Hospital of Shantou University Medical College, Shantou 515041, Guangdong, China.
6. Department of Radiation Oncology, Cancer Hospital of Shantou University Medical College, Shantou 515041, Guangdong, China.
* Can-Tong Liu, Xin-Yi Huang, and Bin-Liang Huang contributed equally to this study.
Abstract
Background: The incidence of esophagogastric junction adenocarcinoma (EJA) patients was increasing but their prognoses were poor. Blood-based predictive biomarkers were associated with prognosis. This study was to build a nomogram based on preoperative clinical laboratory blood biomarkers for predicting prognosis in curatively resected EJA.
Methods: Curatively resected EJA patients, recruited between 2003 and 2017 in the Cancer Hospital of Shantou University Medical College, were divided chronologically into the training (n=465) and validation groups (n=289). Fifty markers, involving sociodemographic characteristics and preoperative clinical laboratory blood indicators, were screened for nomogram construction. Independent predictive factors were selected using Cox regression analysis and then were combined to build a nomogram to predict overall survival (OS).
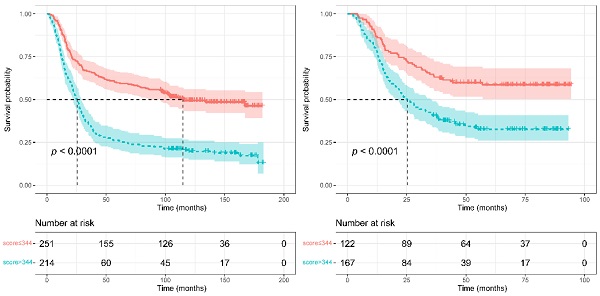
Results: Composed of 12 factors, including age, body mass index, platelets, aspartate aminotransferase-to-alanine transaminase ratio, alkaline phosphatase, albumin, uric acid, IgA, IgG, complement C3, complement factor B and systemic immune-inflammation index, we constructed a novel nomogram for OS prediction. In the training group, when combined with TNM system, it acquired a C-index of 0.71, better than using TNM system only (C-index: 0.62, p < 0.001). When applied in the validation group, the combined C-index was 0.70, also better than using TNM system (C-index: 0.62, p < 0.001). Calibration curves exhibited that the nomogram-predicted probabilities of 5-year OS were both in consistency with the actual 5-year OS in both groups. Kaplan-Meier analysis exhibited that patients with higher nomogram scores contained poorer 5-year OS than those with lower scores (p < 0.0001).
Conclusions: In conclusion, the novel nomogram built based on preoperative blood indicators might be the potential prognosis prediction model of curatively resected EJA.
Keywords: Esophagogastric junction adenocarcinoma, Clinical laboratory blood indicators, Nomogram, Prognosis, Prediction

 Global reach, higher impact
Global reach, higher impact