Impact Factor
ISSN: 1837-9664
J Cancer 2021; 12(17):5331-5337. doi:10.7150/jca.59193 This issue Cite
Research Paper
Prognostic Value of KRAS Exon 3 and Exon 4 Mutations in Colorectal Cancer Patients
1. Department of Colorectal Surgery, Fudan University Shanghai Cancer Center, Shanghai, China.
2. Department of Oncology, Shanghai Medical College, Fudan University, Shanghai, China.
3. Department of Pathology, Fudan University Shanghai Cancer Center, Shanghai, China.
4. Department of Biostatistics and Bioinformatics, Emory University, Atlanta, GA.
*These authors contributed equally to this study.
Abstract
Background: The clinical significance of KRAS exon 3/4 mutations in colorectal cancer (CRC) remains unclear. We aimed to assess the prognostic value of KRAS exons 3 and 4 mutations to determine the necessity for their testing.
Methods: KRAS mutations in exon 2/3/4 were evaluated in 1816 stage I-IV patients with colorectal adenocarcinoma.
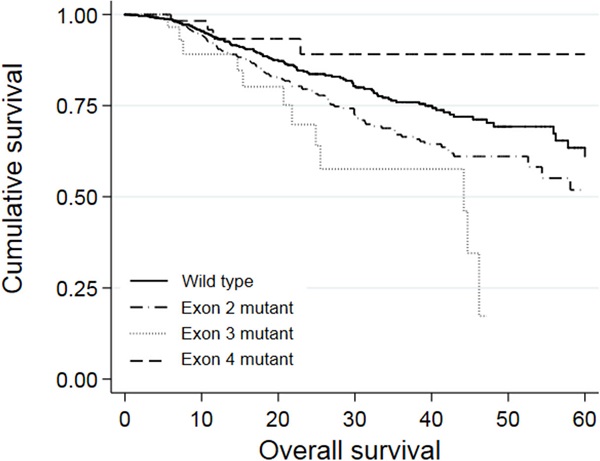
Results: The mutation rates of KRAS and KRAS exons 2, 3, and 4 were 49.0%, 43.0%, 1.9%, and 4.1%, respectively. Univariate survival analysis showed that patients with exon 3 mutation had worse overall survival (OS) compared to those with KRAS exon 2 mutation or wild-type KRAS (P = 0.044, and P = 0.001). Meanwhile, there was no difference in survival between patients with wild-type KRAS and with exon 4 mutation (P = 0.128). In multivariate analysis, KRAS mutations in exon 3 and 2 were both independent factors for worse OS (Exon 3, P = 0.032, HR = 1.861, 95% CI: 1.021-3.391; Exon 2, P = 0.049, HR = 1.298, 95% CI: 1.002-1.682). Among the patients with KRAS exon 2 mutations, those that had mutations in codon 13 had significantly worse prognosis than those with wild-type KRAS (P = 0.001) or KRAS codon 12 mutations (P = 0.003).
Conclusions: In KRAS-mutated CRC, exon 3 mutations predict the worst prognosis, while exon 4 mutations predict the best prognosis. Among KRAS exon 2 mutated patients, codon 13 mutations predict worse prognosis than codon 12 mutations. Mutations of different KRAS exons should be analyzed separately.
Keywords: KRAS exon 3, KRAS exon 4, KRAS mutations, colorectal cancer, clinicopathologic features, prognosis

 Global reach, higher impact
Global reach, higher impact