Impact Factor ISSN: 1837-9664
J Cancer 2021; 12(7):1907-1914. doi:10.7150/jca.53365 This issue Cite
Research Paper
Multidisciplinary team consultation for resectable Gastric Cancer: A propensity score matching analysis
1. Department of Gastrointestinal Surgery, The Sixth Affiliated Hospital, Sun Yat-sen University, Guangzhou, 510655, China.
2. Department of Laboratory Science, The Second Affiliated Hospital, Guangzhou University of Chinese Medicine, Guangzhou, 510105, China.
3. Department of Medical Oncology, The Sixth Affiliated Hospital, Sun Yat-sen University, Guangzhou, 510655, China.
4. Department of Radiology, The Sixth Affiliated Hospital, Sun Yat-sen University, Guangzhou, 510655, China.
5. Department of Pathology, The Sixth Affiliated Hospital, Sun Yat-sen University, Guangzhou, 510655, China.
6. Guangdong Institute of Gastroenterology, Guangdong Provincial Key Laboratory of Colorectal and Pelvic Floor Diseases, Guangzhou, 510655, China.
*These authors contributed equally to this work.
Abstract
Purpose: Previous studies proposed that the multidisciplinary team (MDT) consultation could improve tumor staging accuracy and outcomes of patients with gastric malignancy. However, evidence-based reports remain limited. This study aimed to determine the effectiveness of MDT for tumor staging accuracy and outcomes of patients with resectable gastric cancer, and to explore the potential factors affecting its effectiveness.
Methods: This retrospective study enrolled 719 gastric cancer patients who underwent gastrectomy in our hospital. After propensity score matching, 378 patients were selected, including 189 in the non-MDT group and 189 in the MDT group. Data regarding baseline characteristics, staging, treatments, and survival were analyzed.
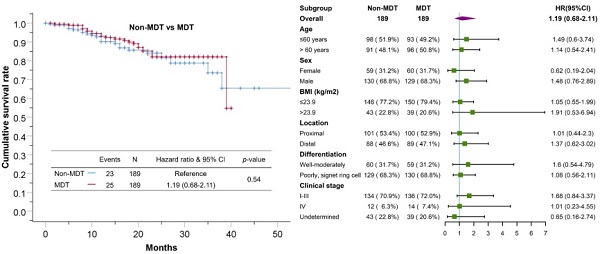
Results: The data showed that the staging accuracy in the MDT group and non-MDT group was comparable (53% vs 61% for T stage, 46.1% vs 35.3% for N stage, and 78.3% vs 78.7% for M stage). The MDT group had a higher proportion of preoperative chemotherapy (39.2% vs 28%, p=0.03) and laparoscopic surgery (82.5% vs 72%, p=0.02) than the non-MDT group. However, the achievement of R0 resection was similar in the two groups (93.7% vs 88.9%, p=0.73). There was no significant difference in the 1-year and 3-year overall survival rates between the two groups. Moreover, we observed poor patient compliance when the MDT recommended further examinations, radiotherapy, or chemotherapy before surgical interventions.
Conclusion: MDT consultation has limited effects on improving the staging accuracy and treatment outcomes including survival of patients with resectable gastric cancer. Poor patient compliance may be a factor affecting the effectiveness of MDT consultation.
Keywords: multidisciplinary team consultation, gastric cancer, propensity score matching, survival, patient compliance

 Global reach, higher impact
Global reach, higher impact