3.2
Impact Factor
ISSN: 1837-9664
J Cancer 2024; 15(11):3531-3538. doi:10.7150/jca.95769 This issue Cite
Research Paper
Influence of High-Risk Pathological Factors and their Interaction on the Survival Benefit of Adjuvant Chemotherapy in Stage II Rectal Cancer: A Retrospective Study
1. School of Medicine, Nankai University, Tianjin, China.
2. Department of Colorectal Surgery, Tianjin Union Medical Center, Tianjin, China.
3. School of Integrative Medicine, Tianjin University of Traditional Chinese Medicine, Tianjin, China.
4. Tianjin Medical University, Tianjin, China.
5. Department of clinical laboratory, Tianjin Union Medical Center, Tianjin, China.
6. The Institute of Translational Medicine, Tianjin Union Medical Center, Tianjin, China.
7. Tianjin Institute of Coloproctology, Tianjin, China.
8. Department of Gastroenterology, Tianjin Union Medical Center, Tianjin, China
9. Department of Immunology, Nankai University School of Medicine, Nankai University, Tianjin, China.
10. Department of General Surgery, The First Affiliated Hospital of Hebei North University, Hebei, China.
11. Tianjin Academy of Traditional Chinese Medicine Affiliated Hospital, Tianjin, China.
*Kailong Zhao, Hongzhou Li, Wenwen Pang, Xuanzhu Zhao contributed equally to this article.
Abstract
Objectives: We investigated the impact of high-risk factors in stage II (TNM stage) rectal cancer patients to determine whether they benefit from adjuvant chemotherapy after surgery. Additionally, we explored the interaction between high-risk factors and adjuvant chemotherapy. Our study provides refined guidance for postoperative treatment in patients with stage II rectal cancer.
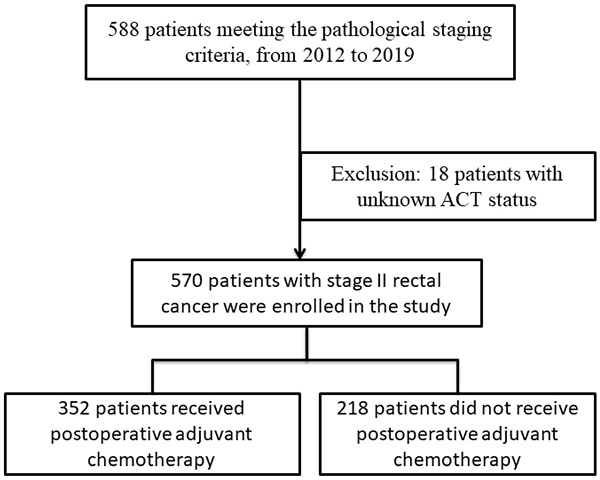
Methods: The retrospective study included 570 stage II rectal adenocarcinoma patients who underwent total mesorectal excision surgery at Tianjin Union Medical Center from August 2012 to July 2019. We employed Cox regression models to assess the collected pathological and clinical factors, identifying the risk factors for overall survival (OS) and disease-free survival (DFS). Additionally, we thoroughly examined the interaction between various high-risk pathological factors and postoperative chemotherapy (ACT), including multiplicative interaction (INTM) and additive interaction (RERI).
Results: Among the 570 stage II rectal cancer patients in this study, the average age was 62 years, with 58.9% (N=336) of the population being older than 60. Males accounted for the majority at 64.9% (N=370). Age was found to have an impact on whether patients received adjuvant chemotherapy after surgery (P<=0.001).Furthermore, age (HR: 1.916, 95% CI: 1.158-3.173, P=0.011; HR: 1.881, 95% CI: 1.111-3.186, P=0.019), TNM stage (HR: 2.216, 95% CI: 1.003-4.897, P=0.029; HR: 2.276, 95% CI: 1.026-5.048, P=0.043), the number of lymph nodes cleared during surgery (HR: 1.968, 95% CI: 1.112-3.483, P=0.017; HR: 1.864, 95% CI: 0.995-3.493, P=0.045), and lymphovascular invasion (HR: 2.864, 95% CI: 1.567-5.232, P=0.001; HR: 3.161, 95% CI: 1.723-5.799, P<0.001) were identified as independent risk factors for patients' overall survival (OS) and disease-free survival (DFS). Moreover, the interaction analysis, both multiplicative and additive, revealed significant interactions between the number of lymph nodes cleared during surgery and the administration of adjuvant chemotherapy. For OS (HR for multiplicative interaction: 0.477, p=0.045; RERI: -0.531, 95% CI: -1.061, -0.002) and for DFS (HR for multiplicative interaction: 0.338, p=0.039; RERI: -1.097, 95% CI: -2.190, -0.005).
Conclusions: This study provides insights into the complex relationship between adjuvant chemotherapy (ACT) and survival outcomes in stage II rectal cancer patients with high-risk pathological factors. The findings suggest that the number of cleared lymph nodes plays a significant role in the efficacy of ACT and underscores the need for individualized treatment decisions in this patient population.
Keywords: Rectal cancer, high-risk factors, interactions, adjuvant chemotherapy

 Global reach, higher impact
Global reach, higher impact