3.2
Impact Factor
ISSN: 1837-9664
J Cancer 2021; 12(8):2275-2284. doi:10.7150/jca.52539 This issue Cite
Research Paper
Prognostic efficacy of the combination of the pretreatment systemic Immune-Inflammation Index and Epstein-Barr virus DNA status in locally advanced Nasopharyngeal Carcinoma Patients
Cancer Center, Union hospital, Tongji Medical College, Huazhong University of Science and Technology, Wuhan 430022, China.
*These authors contributed equally to this study.
Abstract
Background: The systemic immune-inflammation index (SII) and Epstein-Barr virus DNA (EBV DNA) levels has been used as a prognostic marker for nasopharyngeal carcinoma (NPC) patients, but there is no in-depth study in locally advanced NPC patients and no research on the predictive value of their combination. Our study aimed to evaluate the prognostic efficacy of the pretreatment SII, EBV DNA levels and their combination in locally advanced NPC patients receiving induction chemotherapy (IC) followed by concurrent chemoradiotherapy (CCRT).
Materials and methods: 319 patients diagnosed with locally advanced NPC receiving IC followed by CCRT were retrospectively reviewed (213 in the training cohort and 106 in the validation cohort). The cut-off value for the SII was determined using receiver operating characteristic (ROC) curve. Correlations between characteristics of patients were assessed using the Pearson correlation coefficient. Survival curves for the SII, EBV DNA levels and their combination were analyzed using the Kaplan-Meier method and compared using the log-rank test. Univariate and multivariate analyses were performed by the Cox proportional hazards regression model to evaluate the prognostic impact on overall survival (OS) and progression-free survival (PFS). A prognostic nomogram was generated and its prediction ability was measured by the concordance index (C-index).
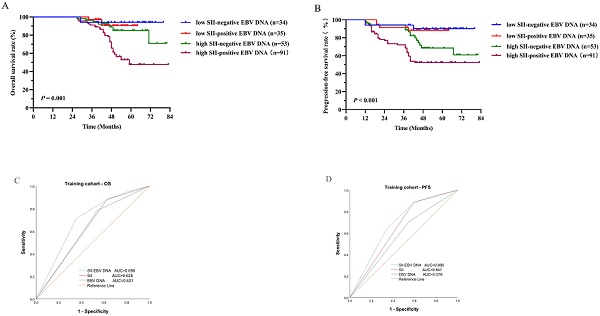
Results: The optimal cutoff point for the SII was 402.10. A higher SII and EBV DNA positivity were demonstrated to be related to poorer survival outcomes (P < 0.05). Multivariate analyses showed that a higher SII, EBV DNA positivity and their combination were powerful independent risk factors for OS and PFS (P < 0.05). The SII - EBV DNA had the largest area under the curve (AUC) compared to either score alone. The incorporation of the SII - EBV DNA into established nomogram achieved higher C-index in the prediction of OS and PFS, indicating its superior for predicting survival. All results were found in the training cohort and confirmed in the validation cohort.
Conclusions: The pretreatment SII and EBV DNA levels are promising factors for predicting survival in locally advanced NPC patients. The combination of them, which was superior to either score alone, was a complement to the conventional TNM staging system.
Keywords: systemic immune-inflammation index, Epstein-Barr virus DNA, locally advanced nasopharyngeal carcinoma, prognosis

 Global reach, higher impact
Global reach, higher impact