3.2
Impact Factor
ISSN: 1837-9664
J Cancer 2022; 13(6):1706-1712. doi:10.7150/jca.63509 This issue Cite
Research Paper
Expression of Prostate-specific Membrane Antigen (PSMA) in Papillary Renal Cell Carcinoma - Overview and Report on a Large Multicenter Cohort
1. Dept. of Medical Oncology, National Center of Tumor Diseases, University Hospital Heidelberg, 69120 Heidelberg, Germany
2. Institute of Pathology, University Hospital Erlangen-Nuernberg, Friedrich Alexander University (FAU), 91054 Erlangen, Germany
3. Department of Urology, University Hospital Münster, 48149 Münster, Germany
4. Department of Urology, University Hospital Göttingen, 37075 Göttingen, Germany
5. Institute of Pathology, University Hospital Göttingen, 37075 Göttingen, Germany
6. Department of Urology and Pediatric Urology, University Hospital Saarland (UKS), 66421 Homburg, Germany
7. Department of Urology, University Hospital Marburg, 35037 Marburg, Germany
8. Department of Urology, University Hospital Munich, 81337 Munich, Germany
9. Department of Urology, University Hospital Heidelberg, 69120 Heidelberg, Germany
10. Institute of Pathology, University Hospital Mainz, 55131 Mainz, Germany
11. Department of Urology and Pediatric Urology, University Hospital Erlangen, 91058 Erlangen, Germany
12. Department of Urology, Marien-Hospital Herne, Ruhr University Bochum, 44625 Herne, Germany
13. Department of Urology, University Hospital Mainz, 55131 Mainz, Germany
14. Department of Urology, University Hospital Frankfurt, 60590 Frankfurt/Main, Germany
15. Department of Urology, University Hospital Regensburg, 93053 Regensburg, Germany
16. Department of Hematology, Hemostasis, Oncology and Stem Cell Transplantation, Hannover Medical School, 30625 Hannover, Germany
17. Present address: Institute of Urology, Prosper-Hospital GmbH, 45659 Recklinghausen, Germany
18. Present address: Urological Group and Clinic Derouet/Pönicke/Becker, Boxberg Centre, 66538 Neunkirchen, Germany
19. Present address: Department of Urology, Asklepios Clinics Altona, 22763 Hamburg, Germany
20. Present address: Institute of Pathology/Gerhard-Domagk Institute, University Hospital Münster, 48149 Münster, Germany
21. Present address: Department of Urology and Pediatric Urology, University Hospital Mainz, 55131 Mainz, Germany
22. Present address: Department of Gynecology, University Hospital Mainz, 55131 Mainz, Germany
23. Present address: Department of Urology, Kreiskliniken Altötting-Burghausen, 84489 Burghausen, Germany
24. Present address: Department of Hematology, Hemostasis, Oncology and Stem Cell Transplantation, Hannover Medical School, Hannover, Germany
†These authors contributed equally to this work.
‡Member of the IAGN (Interdisciplinary working group renal cell cancer, DKG)
§Member of the ICOG-CCC-H (Interdisciplinary CoOperative Immune Oncology Group, Comprehensive Cancer Center, Hannover, Germany).
Abstract
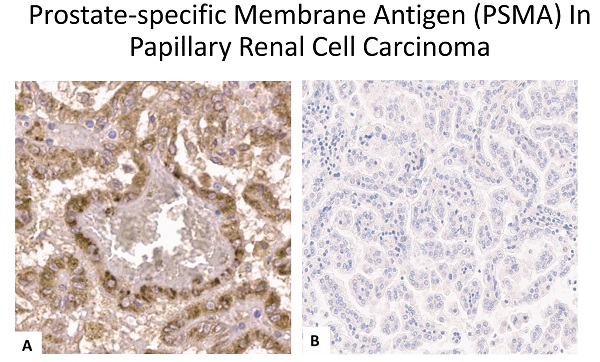
Prostate specific membrane antigen (PSMA) is an emerging diagnostic and therapeutic target in prostate cancer. 68Ga-PSMA-labeled hybrid imaging is used for the detection of prostate primary tumors and metastases. Therapeutic applications such as Lutetium-177 PSMA radionuclide therapy or bispecific antibodies that target PSMA are currently under investigation within clinical trials. The expression of PSMA, however, is not specific to prostate-tissue. It has been described in the neovascular endothelium of different types of cancer such as breast cancer, and clear cell renal cell carcinoma (ccRCC). The aim of this study was to analyze PSMA expression in papillary RCC (pRCC) type 1 and type 2, the most common non-ccRCC subtypes, and to evaluate the potential of PSMA-targeted imaging and treatment in pRCC. Formalin-fixed, paraffin-embedded tissue samples of primary tumors were analyzed for PSMA expression by immunohistochemistry. Out of n=374 pRCC specimens from the multicenter PANZAR consortium, n=197 pRCC type 1 and n=110 type 2 specimens were eligible for analysis and correlated with clinical data. In pRCC type 1 PSMA staining was positive in 4 of 197 (2.0%) samples whereas none (0/110) of the pRCC type 2 samples were positive for PSMA in this large cohort of pRCC patients. No significant PSMA expression was detected in pRCC. Reflecting current clinical evaluation of PMSA expression in RCC do not encourage further analysis in papillary subtypes.
Keywords: prostate specific membrane antigen, papillary renal cell carcinoma, kidney cancer

 Global reach, higher impact
Global reach, higher impact